Clear, Healthy & Confident Skin with Atopic Dermatitis Treatment In Pune
Atopic Dermatitis Treatment In Pune, Atopic dermatitis, also known as eczema, is a chronic skin condition characterized by dry, itchy, inflamed, and sometimes oozing skin. It is a common condition that typically starts in childhood and may continue into adulthood, although it can also develop for the first time in adulthood.
The exact cause of atopic dermatitis is unknown, but it’s believed to affect by a combination of inheritable and environmental factors. People with atopic dermatitis often have a personal or family history of allergies, asthma, or hay fever, suggesting a genetic predisposition.

Symptoms and Causes
Signs & Symptoms of Atopic Dermatitis
- Itchy skin: One of the hallmark symptoms of atopic dermatitis is intense itching. The itching can be severe and persistent, leading to discomfort and sleep disturbances.
- Dry, Sensitive Skin: People with atopic dermatitis often have dry skin that is prone to irritation. The skin may feel rough, scaly, or cracked. The condition commonly affects the face and scalp in infants, while in older children and adults, it often affects the creases of the elbows and knees, wrists, ankles, and neck.
- Rash: Atopic dermatitis typically presents as a rash. The rash can appear as red or brownish-grey patches on the skin. In infants, the rash may ooze fluid and crust over, leading to skin crusting and scaling.
- Inflammation and swelling: The affected skin may become inflamed and swollen. This can give the skin a puffy or swollen appearance.
- Thickened, Leathery Skin: The affected skin may become thickened and leathery in texture with chronic or long-term atopic dermatitis. This is known as lichenification and is a result of persistent scratching or rubbing.
- Skin Infections: Due to the compromised skin barrier and scratching, atopic dermatitis can make the skin more susceptible to infections. Bacterial, viral, or fungal infections can occur, leading to additional symptoms like increased redness, warmth, pain, or discharge from the affected area.


What Are The Causes of Atopic Dermatitis
- Genetics: Individuals with a family history of atopic dermatitis, asthma, or hay fever are more likely to develop the condition.
- Immune system dysfunction: Atopic dermatitis is considered to be an immune-mediated condition.
- Skin Barrier Dysfunction: The skin acts as a barrier, preventing moisture loss and protecting against irritants and allergens.
- Environmental Factors: Various environmental factors can trigger or worsen atopic dermatitis symptoms.
- Allergies And Sensitivities: Atopic dermatitis is commonly associated with other allergic conditions such as asthma, allergic rhinitis (hay fever), or food allergies.
- Psychological Factors: Emotional stress and mental health issues can influence the severity of atopic dermatitis symptoms. Stress can trigger flare-ups or worsen existing symptoms, and the condition can cause psychological distress due to its impact on appearance, discomfort, and sleep disturbances.
What Are The Types Of Atopic Dermatitis
- Infantile Atopic Dermatitis: This type of atopic dermatitis typically occurs in infants and young children. It often starts between 2 and 6 months of age and commonly affects the face, scalp, and extensor surfaces of the arms and legs. The rash is typically red, itchy and may ooze fluid.
- Childhood Atopic Dermatitis: Childhood atopic dermatitis is a condition that persists from infancy into childhood. The rash tends to become more localized and commonly appears in the flexural areas, such as the creases of the elbows and knees. It may also affect the neck, wrists, ankles, and feet. Itching is a prominent symptom.
- Adolescent and Adult Atopic Dermatitis: Atopic dermatitis can continue into adolescence and adulthood, although it may improve or change in presentation. The rash often appears in the same areas as childhood atopic dermatitis but may also extend to the hands, eyelids, and other areas. Itching, dryness, and scaling are characteristic features.
- Hand Eczema: Hand eczema refers to atopic dermatitis primarily affecting the hands. It can be triggered or worsened by frequent hand washing, exposure to irritants or allergens, and repetitive tasks. The skin on the hands becomes dry, red, and may develop cracks or blisters.
- Nummular Eczema: Nummular eczema, also known as discoid eczema or nummular dermatitis, is a type of atopic dermatitis characterized by coin-shaped or oval lesions on the skin. These lesions are typically red, scaly and can be very itchy.
- Seborrheic Dermatitis: Seborrheic dermatitis is a common type of eczema that mainly affects the scalp, face (especially eyebrows and nasolabial folds) and other oily areas of the body. It is characterized by greasy, yellowish scales, redness, and itching.

Atopic Dermatitis Treatment Results Before & After


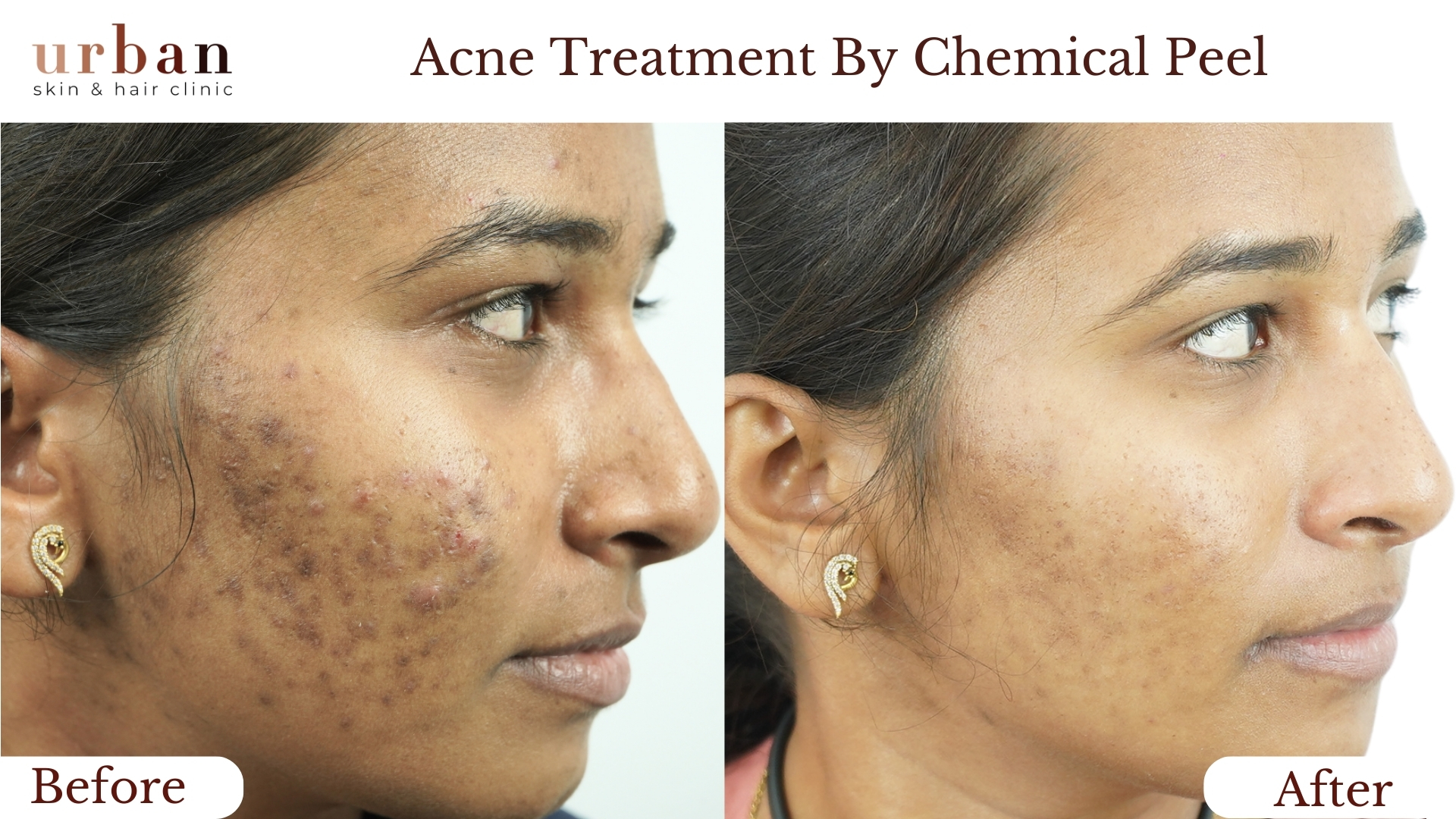
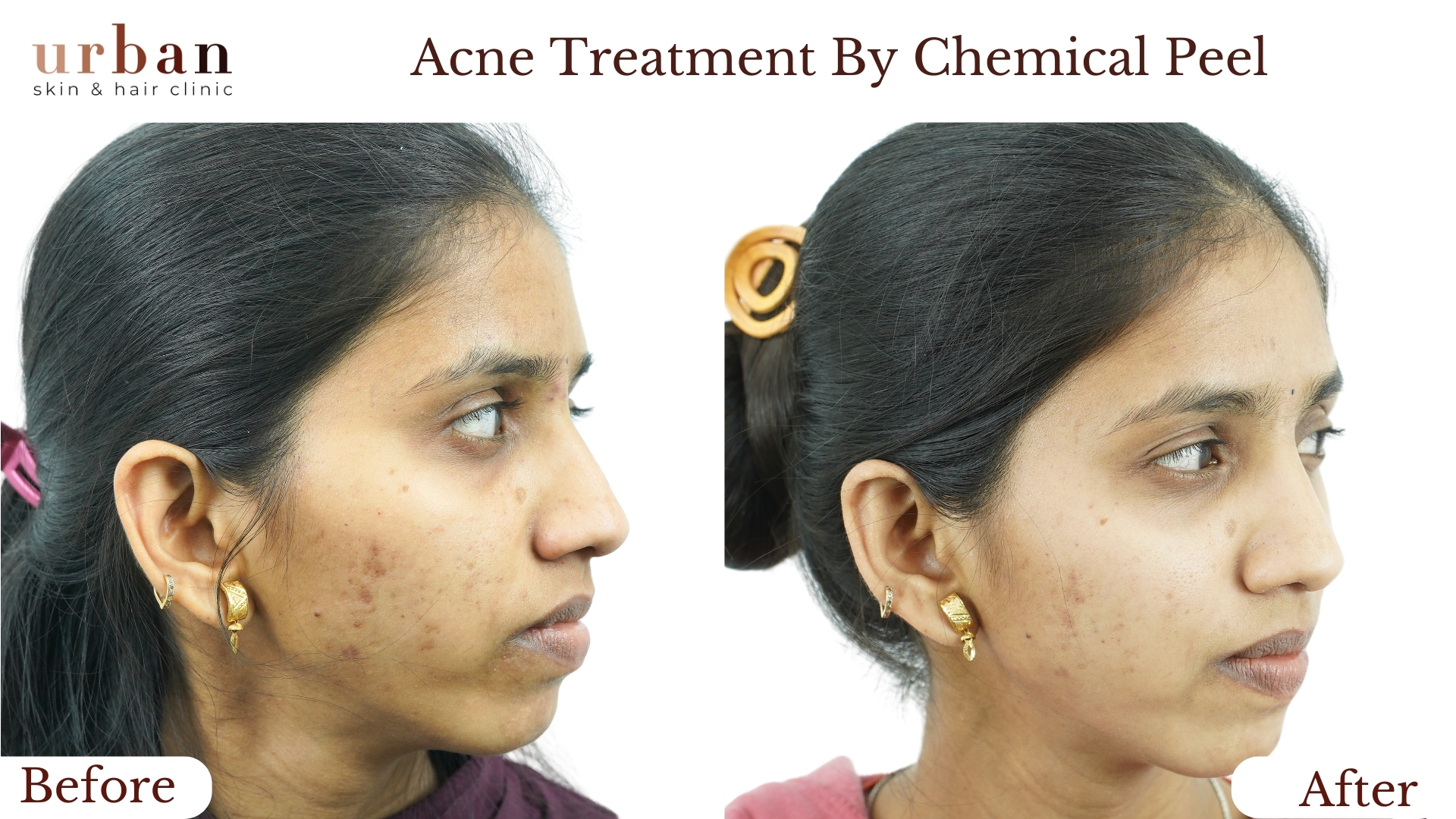
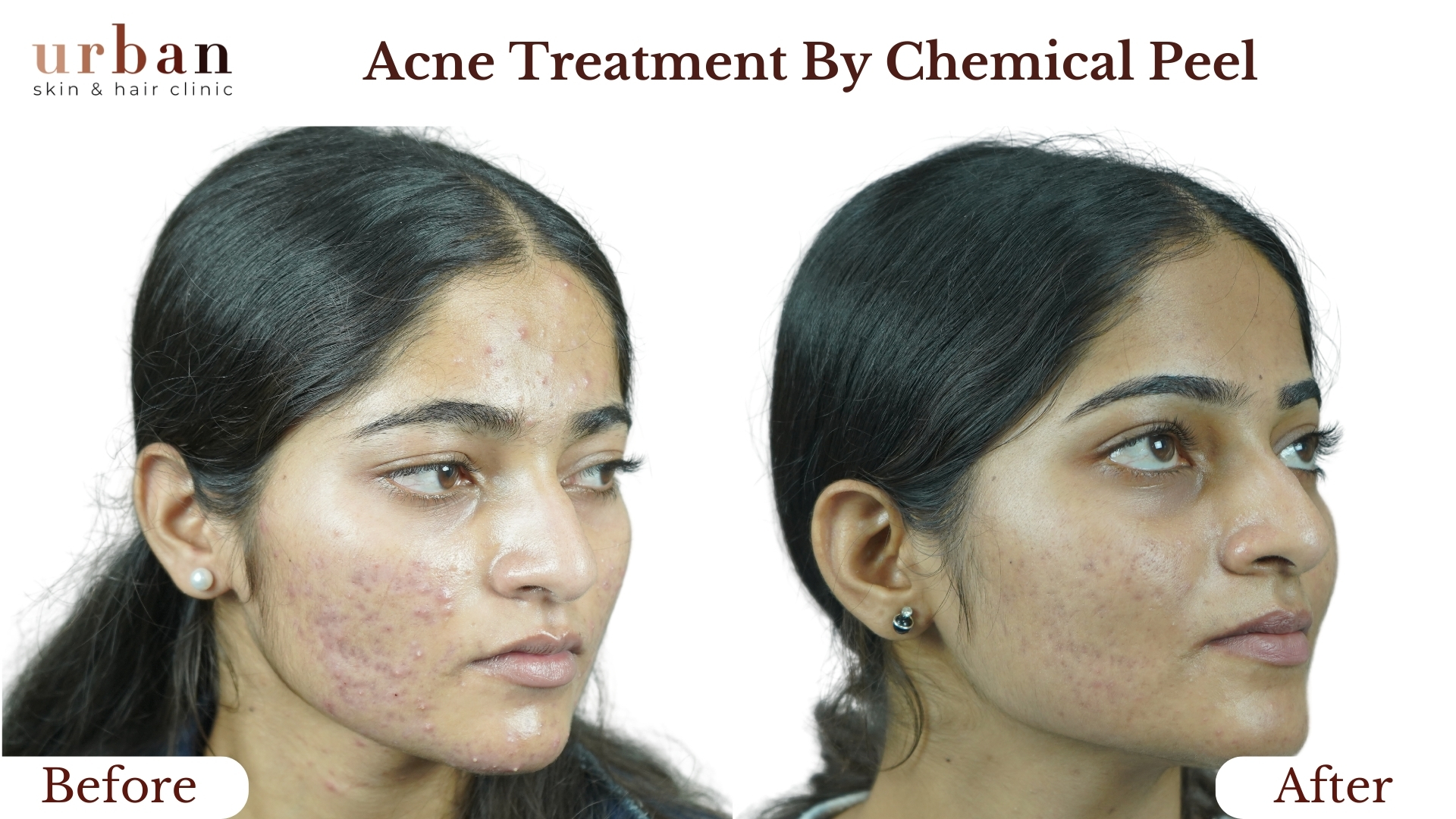
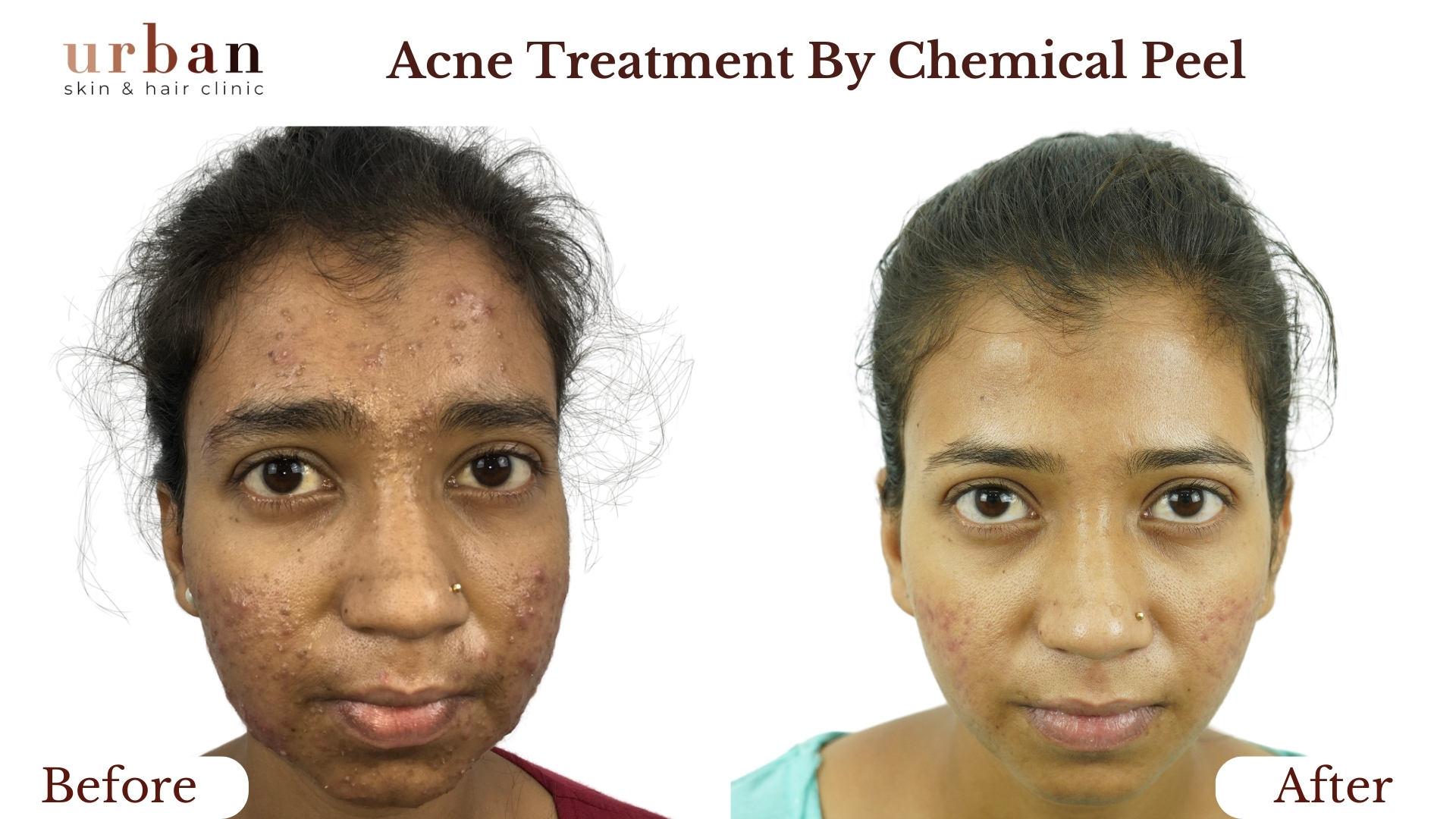
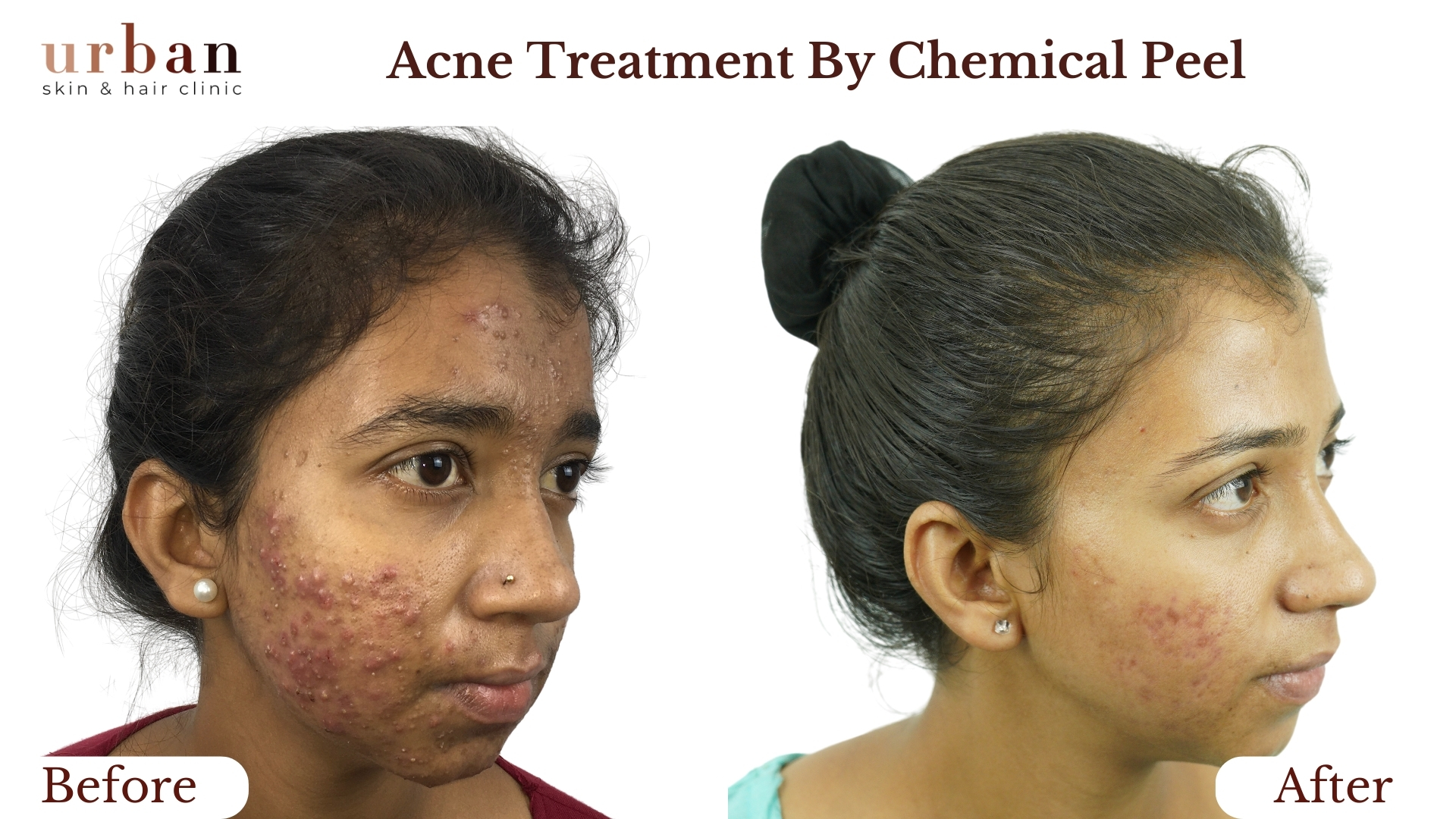
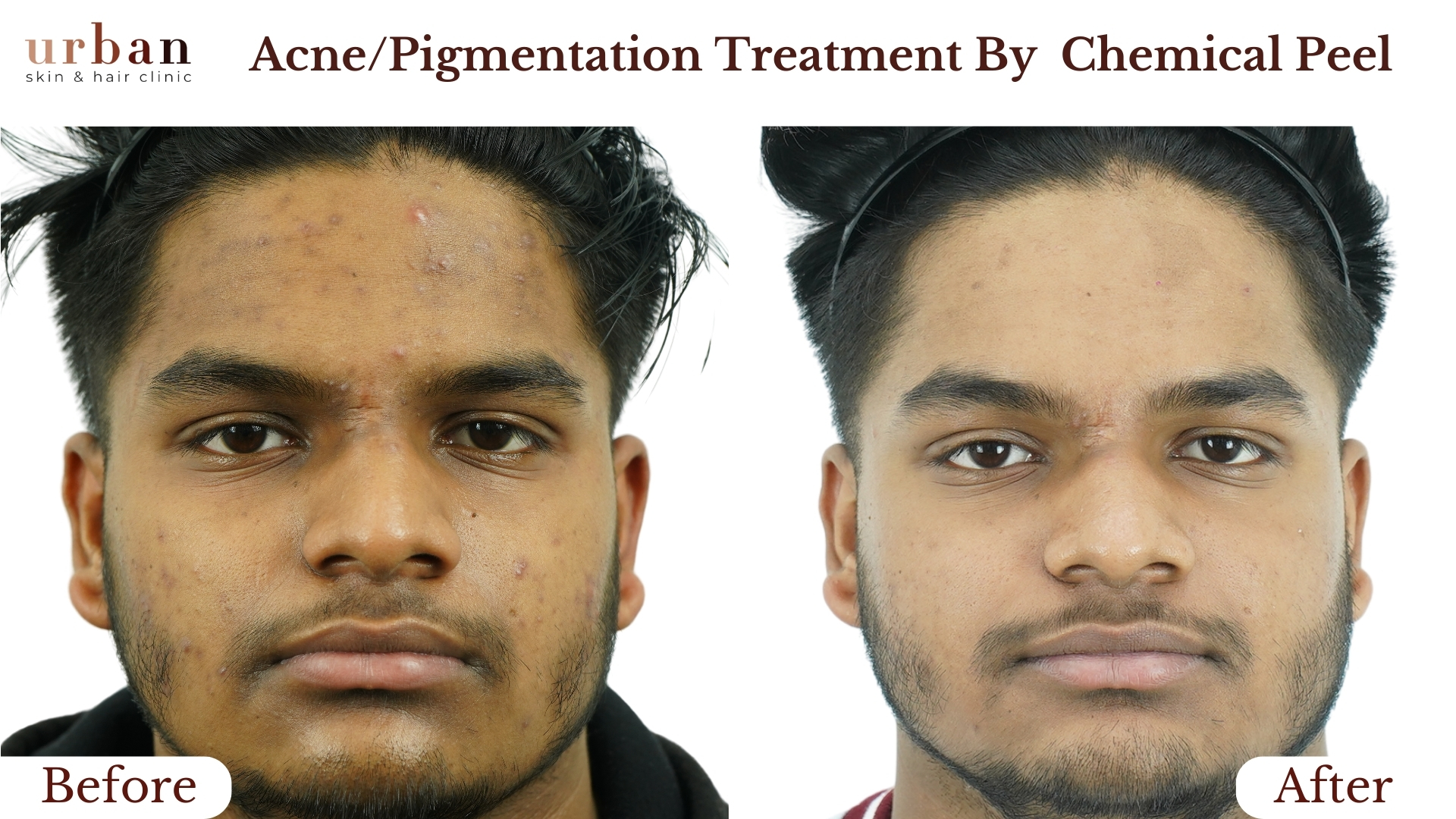
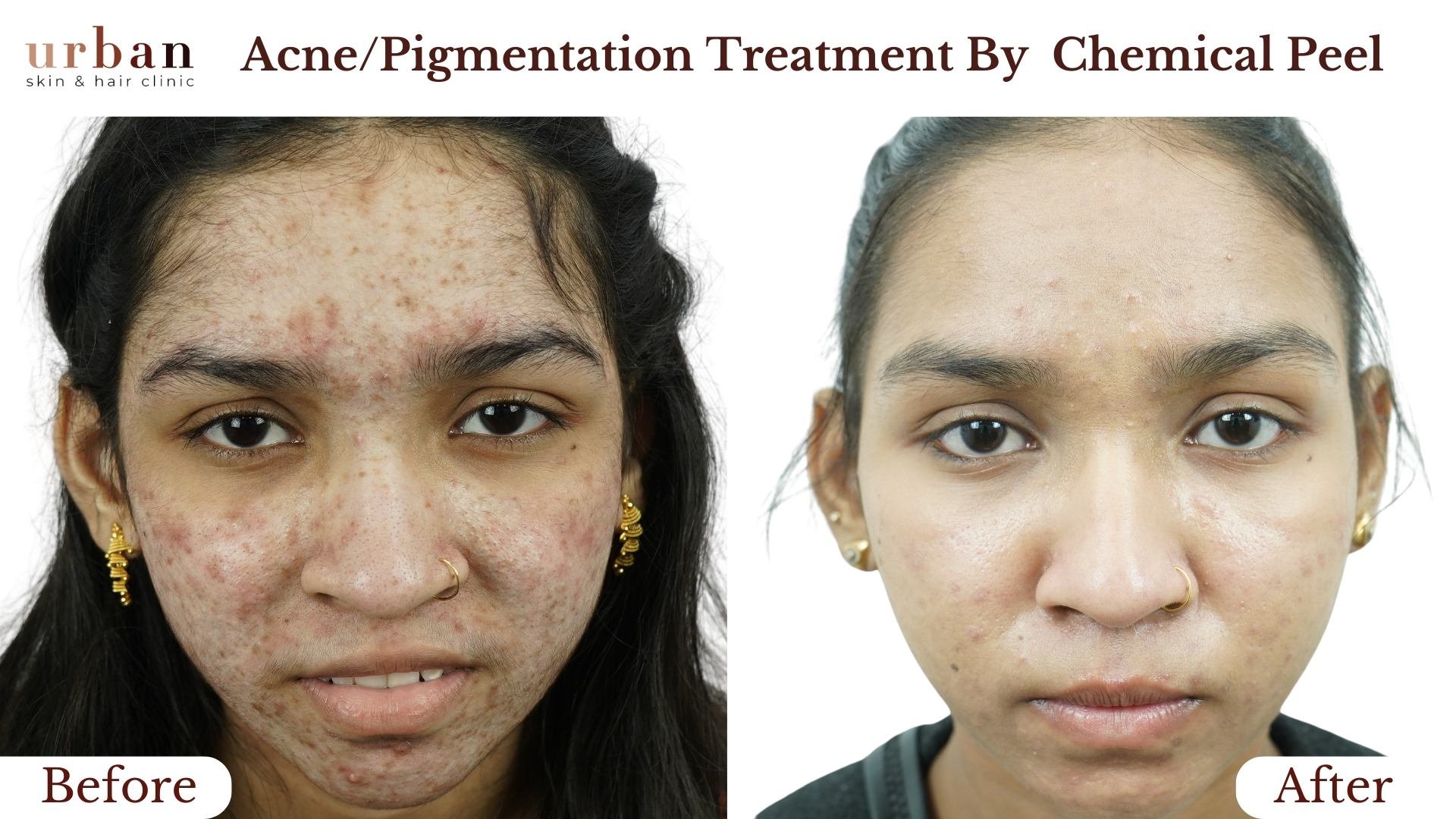

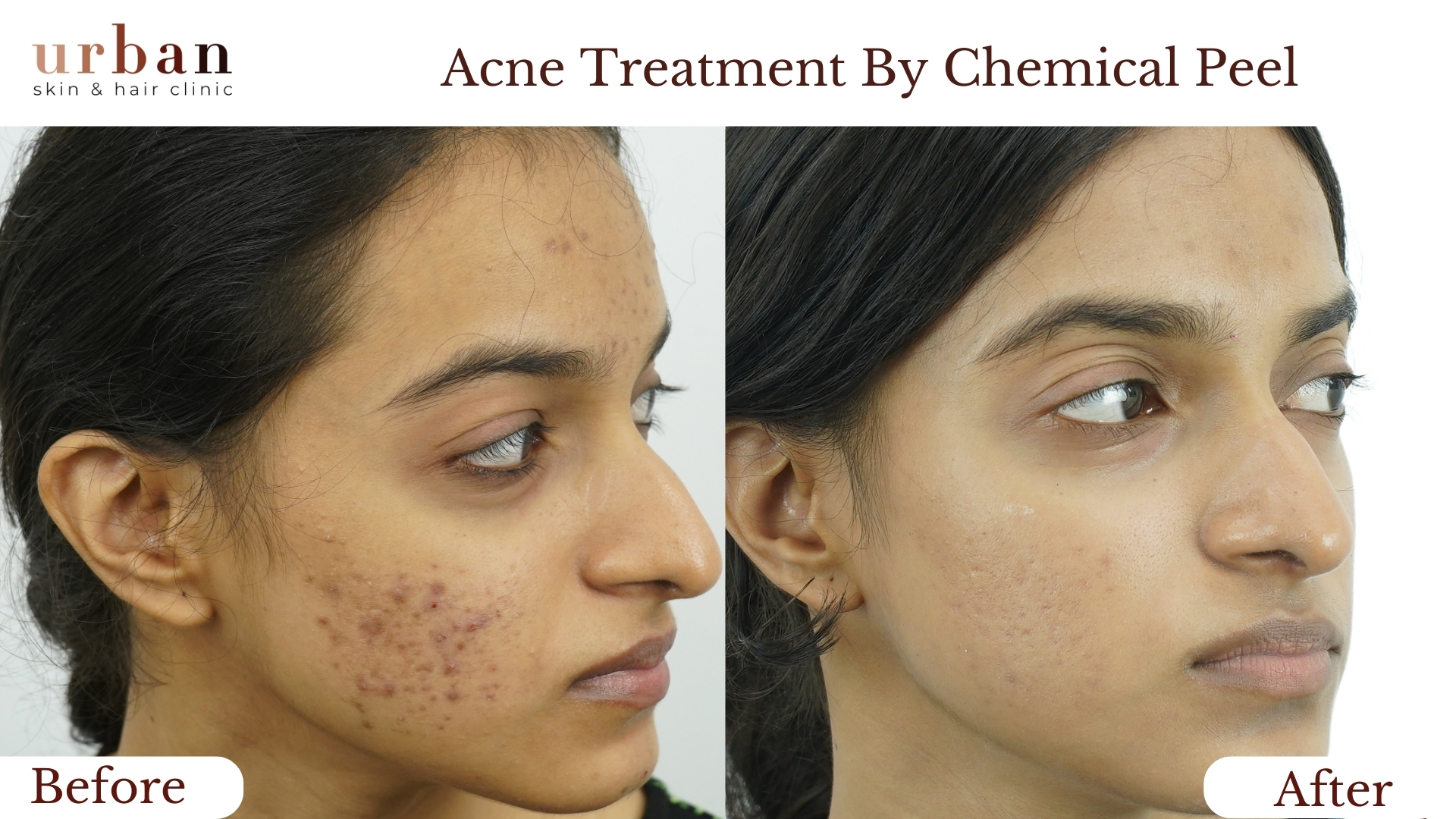
Benefits of Atopic Dermatitis Treatment
Atopic dermatitis treatment controls chronic inflammation and itch, restoring skin barrier function for lasting symptom relief.
Rapid Itch Reduction
Topical corticosteroids and JAK inhibitors like dupilumab reduce pruritus by 70-80% within weeks, breaking the itch-scratch cycle.
Skin Clearance
Biologics achieve EASI-75 (75% improvement) in 50-70% of moderate-severe cases at 16 weeks, clearing plaques effectively.
Flare Prevention
Emollients and calcineurin inhibitors maintain remission, cutting flare frequency by 50% with consistent use.
Quality of Life Gains
Improves sleep, reduces anxiety, and enhances daily function, especially in children with severe atopic dermatitis.

Popular Treatments for Atopic Dermatitis
How To Prevent Atopic Dermatitis?
Here are some precautionary measures that may be helpful:
- Moisturize Regularly: Keeping the skin moisturized is crucial in managing atopic dermatitis. Use gentle, fragrance-free moisturizers or emollients daily to help maintain the skin’s moisture and strengthen the skin barrier.
- Avoid Irritants: Minimize exposure to irritants that can trigger or worsen symptoms. These can include harsh soaps, detergents, fragrances, certain fabrics, and chemicals. Opt for gentle, hypoallergenic products and use fragrance-free laundry detergents and fabric softeners.
- Identify And Avoid Allergens: Allergens can play a role in triggering atopic dermatitis flare-ups. Common allergens include dust mites, pet dander, pollen, certain foods, and mould. If you suspect an allergy, consult an allergist for proper testing and advice on allergen avoidance.
- Maintain A Healthy Environment: Keep your living space clean and dust-free. Regularly vacuum, wash bedding in hot water, and minimize exposure to indoor pollutants and irritants. Maintaining a comfortable humidity level in your home can also help prevent dryness.
- Dress Appropriately: Choose soft, breathable clothing made of natural fibres like cotton or silk. Avoid tight-fitting or rough-textured clothing that can irritate the skin. Be mindful of temperature changes and dress to prevent excessive sweating or overheating.
- Practice Good Skincare Habits: Take lukewarm baths or showers instead of hot ones, as hot water can strip the skin of natural oils. Use mild, fragrance-free cleansers and pat the skin dry with a soft towel rather than rubbing. Apply moisturizer immediately after bathing to lock in moisture.
- Manage Stress: Emotional stress can worsen atopic dermatitis symptoms. Find healthy ways to cope with stress, such as practising relaxation techniques, engaging in regular physical activity, and seeking support from loved ones or professionals if needed.
- Be Cautious With Food Allergies: If you or your child have known food allergies or suspect certain foods may trigger symptoms, work with a healthcare professional to identify and manage them appropriately. They may recommend an elimination diet or specific dietary changes.
- Remember, the effectiveness of preventive measures can vary between individuals.
Consult a Specialist Today
Many of the techniques for preventing pimples may also be used to cure them. Eating well, avoiding stress, and not popping pimples may help manage zits and reduce their length. If your acne continues despite your best efforts, you may need prescription acne treatment. Consult your dermatologist if you’re uncertain about treatment.
FAQ's
Genetic mutations like filaggrin impair skin barrier, combined with immune overactivity and triggers like allergens or irritants, cause inflamed, dry patches.
No, it’s not infectious—it’s driven by immune dysregulation and genetics, not spread by contact.
Many children (60%) improve by adolescence, but adults often have lifelong flares requiring ongoing management.
Certain foods trigger flares in allergic patients; elimination diets help 30% but require medical supervision to avoid malnutrition
Daily emollients repair barrier function, reducing flares by 50% and steroid needs when applied liberally post-bath.