Targeted, Effective & Confidence-Restoring Care for Alopecia Areata
Alopecia Areata causes sudden patchy hair loss and can impact confidence. At Urban Skin and Hair Clinic, we offer advanced alopecia areata treatment in Pune focused on reducing inflammation, reactivating hair follicles, and promoting natural regrowth. Our expert dermatologists in Pune provide personalised treatments including steroid injections, topical immunotherapy, PRP/GFC therapy, and proven hair growth solutions. With accurate diagnosis and customised care, we help you achieve healthier hair and long-term results.
Symptoms and Causes
Symptoms of Alopecia Areata
Alopecia areata is an autoimmune condition that causes sudden and unpredictable hair loss. Common symptoms include:
Round or oval bald patches on the scalp, beard, or other body areas.
Sudden hair shedding in small clumps, often noticed while combing or washing.
Exposed smooth skin where hair has fallen out, without signs of scarring.
Tingling, itching, or mild discomfort in areas before hair loss occurs.
Changes in nails, such as pitting, ridges, or brittleness in some cases.


Causes of Alopecia Areata
Alopecia Areata is an autoimmune hair loss condition where the immune system attacks healthy hair follicles, causing sudden patchy hair loss. If you’re searching for the causes of alopecia areata in Pune or effective hair loss treatment in Pune, understanding these key factors is important:
• Genetics – A family history of autoimmune conditions increases the risk of alopecia areata.
• Immune System Dysfunction – The immune system mistakenly attacks hair follicles, stopping hair growth.
• Stress – Physical or emotional stress is a common trigger for hair loss in many patients in Pune.
• Other Autoimmune Diseases – Conditions like thyroid disorders, vitiligo, or lupus may contribute to alopecia areata.
• Environmental Triggers – Infections, pollution, or allergens can trigger immune responses leading to hair fall.
For those looking for expert alopecia areata treatment in Pune, early diagnosis and personalised care from experienced dermatologists can help manage the condition effectively.

Types of Alopecia Areata
Alopecia areata can affect people in different ways, depending on the extent and location of hair loss. The main types include:
Alopecia Areata (Patchy) – The most common form, where small, round or oval bald patches appear on the scalp or beard.
Alopecia Totalis – Complete loss of hair on the scalp.
Alopecia Universalis – Loss of all body hair, including eyebrows, eyelashes, and body hair.
Diffuse Alopecia Areata – Sudden thinning of hair across the scalp, resembling female or male pattern baldness.
Ophiasis Alopecia – Hair loss in a band-like pattern around the sides and lower back of the scalp.
Before After Results

Problem; alopecia areata
Procedure: mesotherapy
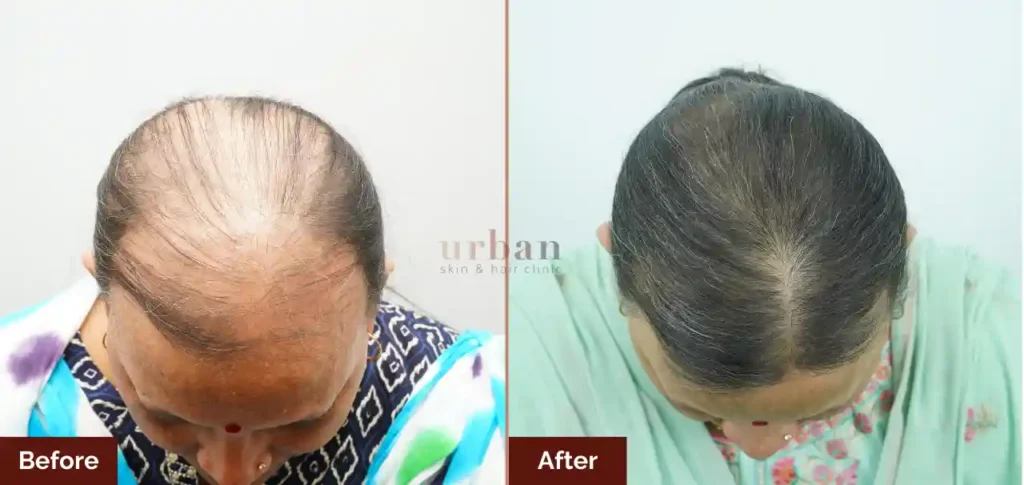
Problem; alopecia areata
Procedure: mesotherapy
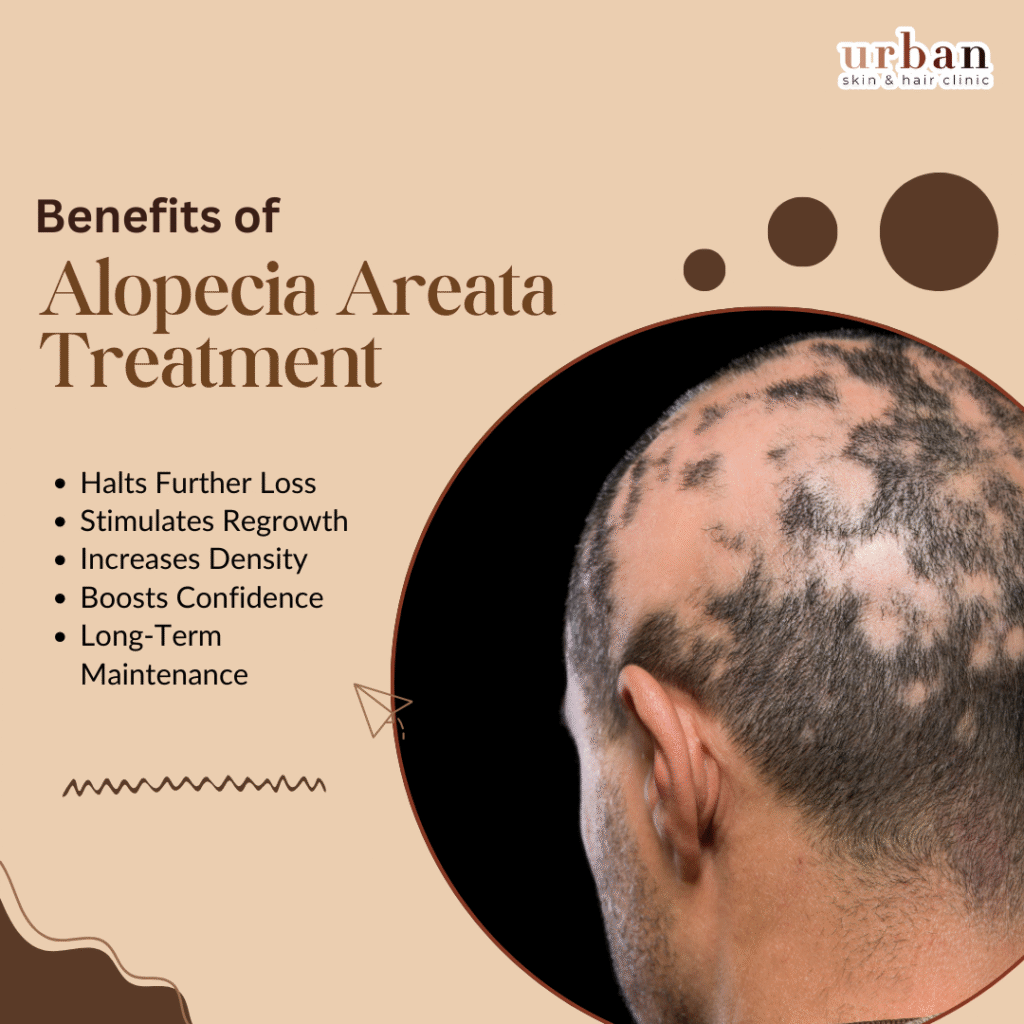
Benefits of Hair Alopecia Areata Treatment
At Urban Skin & Hair Clinic, we provide advanced androgenetic alopecia treatment in Pune to effectively control hair loss and promote natural regrowth.
• Halts Hair Loss: Treatments like finasteride help block DHT, slowing follicle miniaturisation in most men.
• Stimulates Regrowth: Minoxidil improves blood circulation, leading to thicker, healthier hair within a few months.
• Improves Hair Density: PRP therapy in Pune strengthens hair follicles and enhances overall hair volume.
• Boosts Confidence: A restored hairline helps improve self-image and reduces stress-related hair fall.
• Long-Term Results: Combination treatments ensure sustained hair growth and delay further hair loss.
If you’re looking for the best hair loss treatment in Pune, our expert-led, personalised solutions deliver safe and effective results.
Popular Treatments for Alopecia Areata
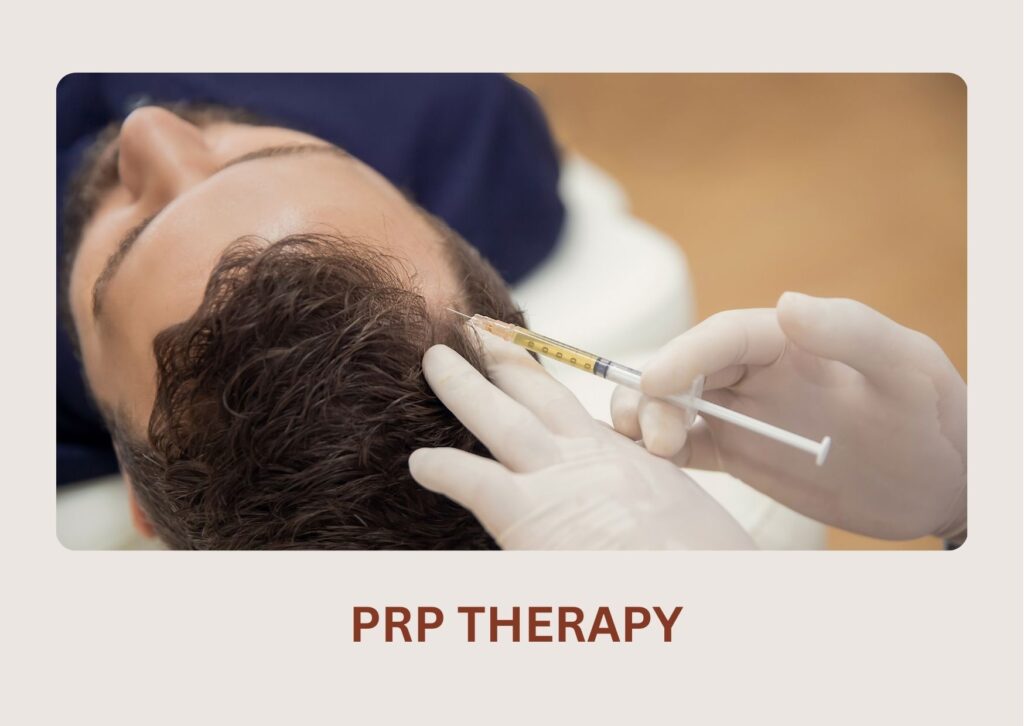
A highly effective treatment where your own growth-factor-rich plasma is injected into the scalp to strengthen follicles, reduce hair fall, and boost regrowth.
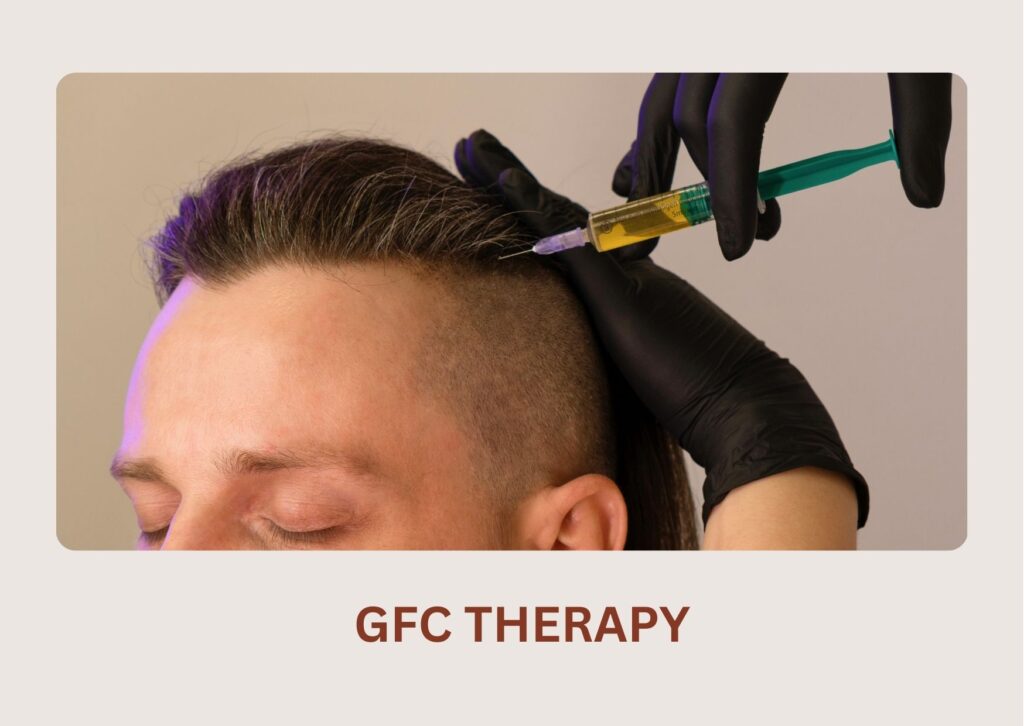
Advanced version of PRP that offers higher growth factor concentration for faster and more noticeable results.
How To Prevent Alopecia Areata?
Alopecia areata, an autoimmune condition causing patchy hair loss, cannot be fully prevented due to its genetic and unpredictable triggers, but lifestyle measures can reduce flare risks and limit spread. Early intervention and stress management prove most effective for those with family history or prior episodes.
Stress Management
Reduce stress through yoga, meditation, or 7-8 hours of nightly sleep, as it triggers immune attacks on follicles. Daily exercise and setting boundaries on commitments help maintain hormonal balance and lower cortisol levels.
Nutrition Support
Consume a balanced diet rich in vitamin D, iron, zinc, protein, and biotin from sources like eggs, spinach, nuts, and fatty fish to bolster follicle health. Address deficiencies early via blood tests, especially relevant for women’s hormonal patterns.
Scalp Care Practices
Maintain gentle hygiene with sulfate-free shampoos, avoiding tight hairstyles, heat tools, or harsh chemicals that strain follicles. Protect scalp from sun with hats or SPF and shield from cold to prevent added damage.
Additional Habits
Quit smoking and prioritize quality sleep, as lifestyle factors like obesity or poor rest may worsen progression. Consult dermatologists at clinics like Urban Skin Hair Clinic for personalized screening and preventive therapies such as PRP.
Consult a Specialist Today
However, if your acne persists despite these efforts, professional acne treatment in Pune may be required. Consulting an experienced dermatologist in Pune can help you choose the right prescription treatments and achieve clearer, healthier skin.
FAQ's
Not always. In many cases, hair grows back within months, but some people may experience repeated cycles of hair loss and regrowth.
It is an autoimmune condition. Stress, genetics, and other autoimmune diseases like thyroid disorders can act as triggers.
There is no permanent cure, but treatments like corticosteroids, minoxidil, and immunotherapy can help control the condition and encourage regrowth.
No, it mainly affects hair and sometimes nails, but it does not impact general physical health.
If you notice sudden patchy hair loss, thinning, or nail changes, consult a dermatologist for early diagnosis and treatment.
What is Alopecia Areata?
Alopecia Areata is an autoimmune disorder where the immune system mistakenly attacks the hair follicles, leading to hair loss in small, round patches. The condition can affect any part of the body, but it’s most commonly seen on the scalp and face. The severity varies: some experience only a few patches of hair loss, while others may suffer from complete scalp hair loss (Alopecia Totalis) or even total body hair loss (Alopecia Universalis).
Causes of Alopecia Areata
The exact cause of Alopecia Areata is not fully understood, but several factors contribute to its development:
- Autoimmune Response: The immune system targets hair follicles as though they are foreign invaders, leading to hair loss.
- Genetics: A family history of autoimmune diseases or Alopecia Areata increases the risk.
- Stress: Emotional or physical stress is believed to trigger or worsen hair loss in some cases.
- Hormonal Imbalances: Conditions like thyroid disease can increase susceptibility to Alopecia Areata.
- Infections or Viral Illnesses: Certain viral infections have been linked to autoimmune responses that cause hair loss.
- Environmental Factors: Pollutants and toxins may trigger flare-ups in those genetically predisposed.

Treatment Benefits
- ✅ Stimulates Hair Regrowth: Aims to activate dormant follicles and regenerate hair growth
- ✅ Reduces Inflammation: Calms the immune response and prevents further damage to follicles
- ✅ Strengthens Hair and Roots: Promotes the growth of thicker, stronger hair strands
- ✅ Prevents Future Hair Loss: Helps stabilize hair regrowth and reduces the risk of recurrence
- ✅ Non-Surgical Options: Safe, non-invasive treatments with minimal downtime
- ✅ Suitable for All Ages and Severity Levels: From patchy hair loss to more extensive cases
- ✅ Improves Scalp Health: Enhances overall scalp nourishment for healthier hair
Before-After Results
Patients typically notice the regrowth of fine hair in the affected areas within 3–6 months of treatment. The density and thickness of the regrown hair improve with ongoing sessions, and many patients experience long-term hair restoration with proper care. Our dermatologists track progress through before-and-after photos to document hair restoration.
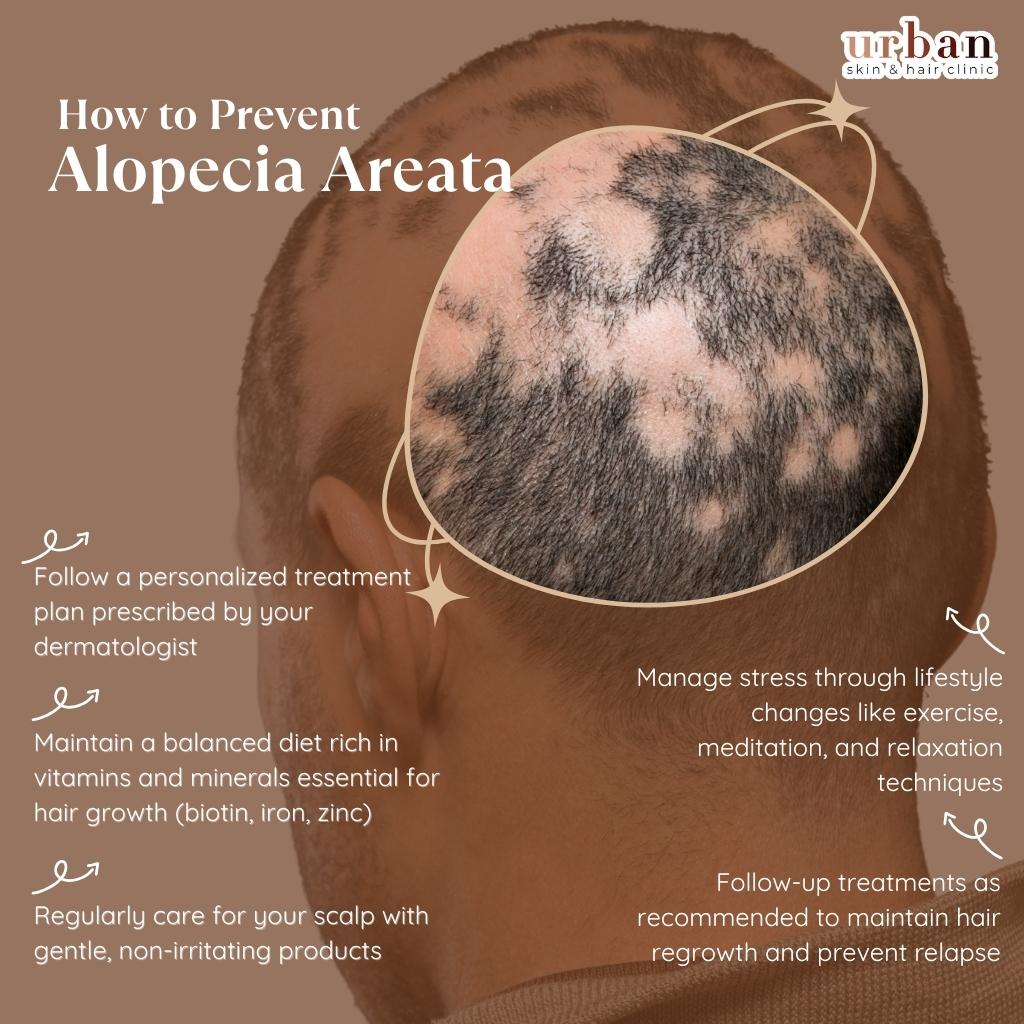
How to Prevent Alopecia Areata Recurrence
- Follow a personalized treatment plan prescribed by your dermatologist
- Manage stress through lifestyle changes like exercise, meditation, and relaxation techniques
- Maintain a balanced diet rich in vitamins and minerals essential for hair growth (biotin, iron, zinc)
- Regularly care for your scalp with gentle, non-irritating products
- Avoid harsh chemical treatments, heat styling, and tight hairstyles
- Follow-up treatments as recommended to maintain hair regrowth and prevent relapse
At Urban Skin and Hair Clinic, we offer a variety of treatments designed to manage and treat Alopecia Areata effectively:
- Steroid Injections: Administered directly into the affected areas to reduce inflammation and promote hair regrowth
- Topical Steroid Creams: Applied to patches of hair loss to encourage follicular activity
- PRP Therapy (Platelet-Rich Plasma): Stimulates hair follicles and promotes healing of the scalp
- Micro needling: Creates micro-injuries on the scalp to encourage hair regrowth by enhancing nutrient absorption
- Mesotherapy: Delivers essential nutrients directly into the scalp to strengthen hair follicles
- Low-Level Laser Therapy (LLLT): Stimulates hair follicles and improves blood circulation in the scalp
- Oral Medications: Prescription options for autoimmune response regulation, such as corticosteroids or immune system modulators
Each treatment is tailored to the patient’s needs, taking into account the severity of the condition and the patient’s health history.
Treatment Options at Urban Skin and Hair Clinic

Meet Our Expert Dermatologist
Dr. Kiran Chotaliya, M.D. Dermatology, is an expert in autoimmune hair loss treatments, including Alopecia Areata. With a compassionate approach and extensive clinical experience, Dr. Kiran will guide you through every step of the treatment process to ensure the best possible outcome.
Alopecia Areata Treatment FAQ
While there is no permanent cure, Alopecia Areata can be effectively managed, and hair regrowth is possible with the right treatments.
Hair regrowth typically begins in 3–6 months, with ongoing treatments recommended to ensure lasting results.
Yes, when administered by a qualified dermatologist, steroid injections are safe and effective for Alopecia Areata.
Yes, it can cause hair loss on the scalp, face (eyebrows, eyelashes), and even the body (Alopecia Universalis). Treatment will be adjusted based on the severity and area affected.